Aspirin was already known to reduce the likelihood of developing colon, esophageal, lung, and prostate cancers. Now, add pancreatic cancer to the list…
The mechanism by which low dose chronic aspirin therapy works is by reducing inflammation. Chronic inflammation is a cancer promoter, that is, it sets conditions necessary for mutations to occur (proliferation) and establishes the environment for heterotypic cellular interactions with inflammatory cells that help to induce the cancer phenotype and then drive cancer development.
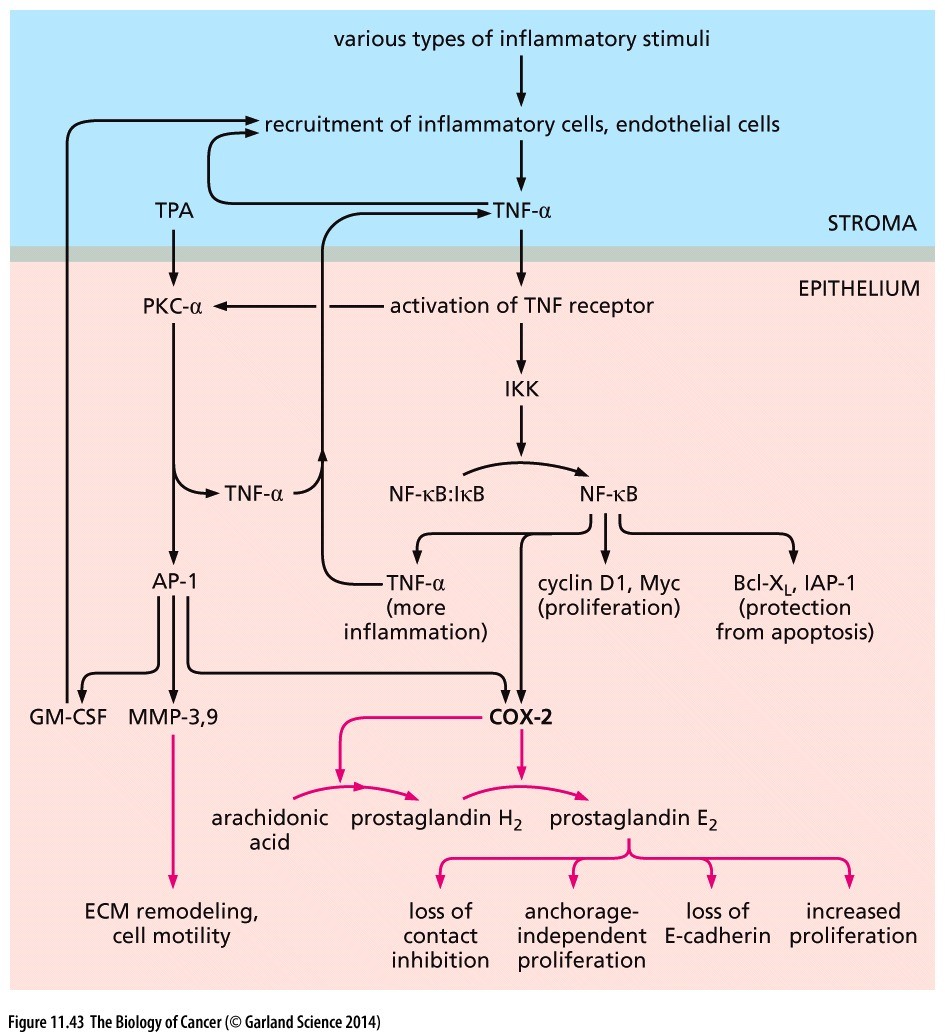
Inflammatory cells secrete TNF (tumor necrosis factor), which induces protein kinase C (PKC), which induces AP-1 and cyclin D-1 leading to proliferation and p53 blockade via mdm2 induction. TNF directly induces NFkB, which is also indirectly induced by PKC. NFkB is a real bad actor, inducing inhibitors of apoptosis, cyclin D, and myc, which induces telomerase, leading to immortalization. As if that weren’t enough, NFkB also induces COX-2, which induces Prostaglanding E-2. PGE2 promotes EMT, loss of contact inhibition, more proliferation, and blocks apoptosis. Aspirin blocks the production of PGE2. See diagram – Copyright 2014 from The Biology of Cancer, 2nd Ed. by Weinberg. Reproduced by permission of Garland Science/Taylor & Francis LLC.
Chronic inflammation also releases reactive oxygen and reactive nitrogen species, which cause DNA damage leading to mutations. (See journal article – Why Cancer and Inflammation.)
In this study, the risk of developing pancreatic cancer reduced by 48%. Of course, aspirin therapy poses risks, as well, notably bleeding and gastric and esophageal ulcers.